|
ALLERGY TESTING:
- Audiometry
- Tympanometry
- Adv Audiology
- Vestibular
- Allergy Testing
- Tinnitus
- Hyperacusis
- Misc. Audiology
- Clinical Photography
 Allergies can be described as an
exaggerated reaction of the immune
system. This is described as a hypersensitivity to specific substances
medically. Allergies can occur in different areas of the body, but
mainly the respiratory system (e.g. hay fever, asthma),
gastro-intestinal tract (e.g. peanut allergies) or the skin (e.g.
contact dermatitis). Allergies can be described as an
exaggerated reaction of the immune
system. This is described as a hypersensitivity to specific substances
medically. Allergies can occur in different areas of the body, but
mainly the respiratory system (e.g. hay fever, asthma),
gastro-intestinal tract (e.g. peanut allergies) or the skin (e.g.
contact dermatitis).
Determining the cause of a
person's allergy will usually start with a consultation with a
specialist taking a clinical history and sometimes completing a
questionnaire. Important clues can be gained by determining known
triggers such as if there are certain times of the year a person is
most affected, certain animals, food types or drug allergies.
From the answers obtained by the questionnaire and history taking the
clinician can then decide whether an allergy skin prick test is
necessary and if testing is needed, just what allergies to test for.
Sometimes it may be more appropriate to take a blood sample and request
a blood test such as radioallergosorbent test (RAST) for things like
atopic dermatitis, the disadvantage of this is that there may be a
delay of more than a week for the results, whereas with skin prick
testing the results will be known that day. There are additional
investigations that can be done with blood samples and this are
described below.
If a skin prick test is indicated then the subject may need to come
back on another day if they are or have been taking antihistamines as
this will suppress their allergic symptoms and inhibit the skin prick
results. Depending on the type of antihistamine determines how long the
wait is before skin prick testing can be done.
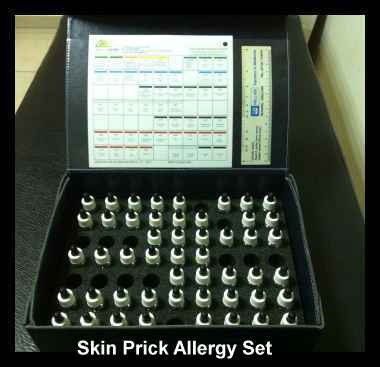
Skin
Prick Testing
Prior to
the start of the skin prick test the skin is cleaned, usually with
alcohol. The forearm is generally used as a location for the drops to
be placed but for children the back can be used. Small drops of
allergens are placed on the skin and labelled. Additionally a positive
and negative control is tested as well.
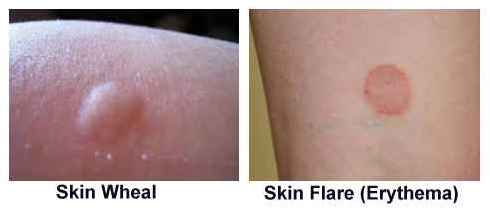 Once the drops are placed
a small lancet is used to prick the skin
through the allergen, no blood is drawn but a slight graze is formed
that allows the allergen to enter the skin. If there is an allergy, it
is caused by specialised immune cells causing a hypersensitive reaction
to the allergen and releases chemicals that cause inflammation. The
result can be seen on the skin as a red patch on the skin called an
erythema or flare or if there is more of a reaction a raised patch of
inflammation is also seen called a wheal Once the drops are placed
a small lancet is used to prick the skin
through the allergen, no blood is drawn but a slight graze is formed
that allows the allergen to enter the skin. If there is an allergy, it
is caused by specialised immune cells causing a hypersensitive reaction
to the allergen and releases chemicals that cause inflammation. The
result can be seen on the skin as a red patch on the skin called an
erythema or flare or if there is more of a reaction a raised patch of
inflammation is also seen called a wheal
15
minutes after the actual skin pricks the reactions to each allergen of
inspected and compared in size to the positive and negative controls.
If the reaction is the same size or smaller than the negative control
then the person is not allergic to that allergen. If the skin reaction
is larger than the negative then the allergic reaction may be scored.
Skin prick testing is a very simple and quick way to determine
allergies. A patient's allergy can be confirmed quickly and the
appropriate advice or treatment implemented. After skin prick testing
the patient can usually be told what they are allergic to and with that
knowledge they may be able to adopt strategies to avoid them in the
future, or they can be assured that they are on the correct treatment
appropriate for their allergy.
Blood Sample
Testing
Blood
testing is another common way to measure the potential for an allergy.
Blood testing should be seen as complimentary to skin prick testing and
not equivalent to it. An advantage of blood testing is that there is no
risk that the test will trigger a severe reaction. Even though the
likelihood of a severe anaphylaxis reaction is very remote in skin
prick testing blood testing is considered the safer option. This is of
note to known higher risk subjects with a life-threatening anaphylactic
reaction or for those that have other destabilising conditions such as
asthma or heart disease..
There are numerous blood testing methods but essentially these tests
look for IgE antibodies in your blood that are specific to a certain
food or other allergen. The higher the level of IgE, the more likely
there is an allergy to that particular allergen.
Radioallergosorbent or
RAST testing used to be the commonest blood test for helping to
diagnose an allergy by using radioimmunoassay to detect specific IgE
antibodies. RAST results are usually scored on a scale of 1 to 6, with
1 being absent or undetectable allergen specific IgE levels and 6 being
an extremely high level of IgE. This is based on the IgE antibody
concentration (kUA/l) ranging from
<0.35 kUA/l to >100 kUA/l. However, newer
allergy blood tests are now available and RAST has generally been
replaced with a superior test called ImmunoCAP Specific IgE Blood Test.
ImmunoCAP is now the
mainastay of blodd testing and superceded the RAST test. Although
similar in principle ImmunoCAP uses an enzyme instead of an isotope to
detect specific IgE antibodies. ImmunoCAP is also quicker to perform
and has a higher sensitivity than it's predecessor, with it's range
from 0.1kUA/l
to >100 kUA/l.
Basophil Activation test is
another blood test but is looking at the activation of Basophils, that
will release chemical mediators if sensitised to an allergen. When
activated the basophil membrane will show specific molecules (CD63 or
CD203c) that allows for the identification of activation. This test is
relatively new and somewhat more laborious and so is not widely
available. Additionally the number of allergens are not as plentiful as
other tests.
Allergen Component Resolved
Diagnostic testing is a new methodology, used mainly for food
allergy diagnosis but the allergen types available are increasing.
Instead of using crude allergen extracts this method uses pure allergen
molecules that are acquired from natural allergen sources or produced
by recombinant expression of allergen encoding cDNA's. The binding of
IgE to these specific proteins can then be assessed. This can then
enable the clinician to distinguish between the different phenotypes of
cross-reactive proteins such as shrimp allergy with dust mite and
cockroach.
There are a number of other 'Allergy Tests' that have never been fully
validated, peer reviewed or proved to be safe and effective.
ELISA test. This measures the IgG and IgG4 antibodies but these is no
convincing evidence to suggest this test has any diagnostic value.
Leucocytotoxic Test. Also know as Bryan's Test as it was developed by
AP Black and further promoted by WT & MP Bryan. This test eluded to
the fact that a patients white blood cells would swell if mixed with a
sensitive allergen. The swelling was then measured and if the
measurement reached a certain threshold a positive response was
recorded. This test was deemed ineffective and without scientific basis
according to Food and Drug Administration (FDA) in USA and to date no
studies have shown any correlation between this test and allergies. The
test has since been remarketed under the name of 'Nutron'.
Hair Analysis. Here, the hair is tested for levels of heavy metals and
then deficiencies in Zinc, Selenium, Chromium, Magnesium and Manganese.
However there is no evidence to support the theory of the relationship
between heavy metals and allergy.
There are many other Alternative or Complementary Health methods of
assessing allergies and caution must be taken where non-approved or
anecdotal evidence is used to justify these methods.

|
|